Labour pain is complex and multifaceted, existing within an individual perception and context, and arising from individual physiology, psychology and cultural perspectives. Notions of ‘normal labour’ differ depending on cultural background, spiritual practice and a woman's phenomenological experiences (Karlsdottir et al, 2014). The International Association for the Study of Pain (IASP, 2014) defines pain as ‘an unpleasant sensory and emotional experience associated with actual or potential tissue damage’—a distinction from the physiological normal role of pain in a birthing context, which may be challenging for both women's perception and midwifery facilitation (Sanders, 2015). The National Institute for Health and Care Excellence (NICE, 2016) prompts practitioners to reflect on how midwives’ ideologies and beliefs influence how women are supported to handle the experience of labour discomfort (Nursing and Midwifery Council (NMC), 2015; Leap and Hunter, 2016). This article focuses on midwives' capacity, through understanding non-pharmacological strategies, to facilitate practice based on ‘working with pain’ (Leap, 1997) rather than ‘pain relief’.
It is crucial that midwives provide holistic and individualised care in supporting women through the pregnancy journey toward the experience of birth. This article will consider how non-pharmacological pain management strategies can be utilised by women and supported by midwives assisting women and their families to experience the wide spectrum of the labour experience without the use of pharmacological agents.
The physiology of pain
Pain is usually considered within the realm of a pathological situation, with connotations of distress and suffering (Simkin and Bolding, 2004; Simkin and Ancheta, 2011a). Many women report concerns during the antenatal period about how they will ‘cope’ with the pain of labour, often feeling unprepared for the experience of birth (Lally et al, 2008), while others report feeling empowered and proud of their birthing ability (Klomp et al, 2014).
As the functionality of pain is predominantly one of protection and warning (Dick-Read, 2013), labour pain must be differentiated from pathological connotations, necessitating midwives to redefine it in the context of normal physiological birth (Walsh, 2012). The quality and intensity of discomfort during the process of labour can vary dramatically, and requires support and reassurance to enable women to respond with confidence to the unknown experience of labour. NICE acknowledges that midwives' own ideologies surrounding pain management require reflection, having the capacity to influence women in their birthing space (NICE, 2016; Leap and Hunter, 2016). Some research suggests a strong midwifery preference for non-pharmacological strategies (Madden et al, 2013).
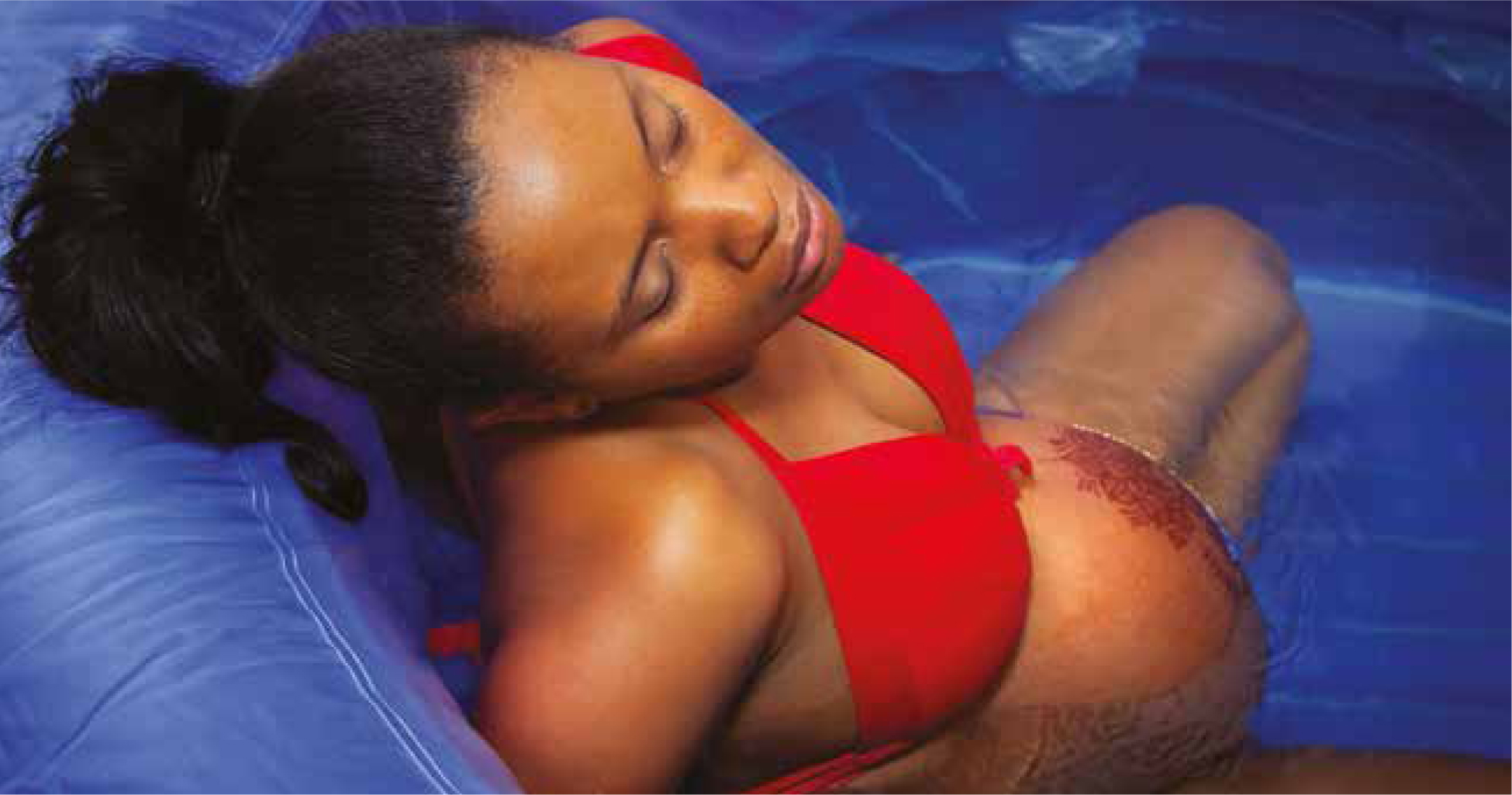 The use of water immersion in birth has been part of national recommendations in the UK since 1993
The use of water immersion in birth has been part of national recommendations in the UK since 1993
With many women reporting their desire to birth without pharmacological assistance (Care Quality Commission, 2013), sharing information during pregnancy about the physical, psychological and dynamic hormonal interplay during labour can avoid the disparity that women report feeling following birth (Lally et al, 2008). Many women acknowledge the place of discomfort in labour, anticipating this as an inherent part of becoming a mother; some report that they prefer models of care based on continuous support and a professional attitude, which accepts that pain is part of birth (Van der Gucht and Lewis, 2015). This is supported by the understanding that the efficacy of pain relief does not result in improved maternal satisfaction; rather, social models of care increase satisfaction, with long-lasting effects on the family unit (Hodnett et al, 2011).
Throughout labour, pain manifests as visceral discomfort from nociceptors in the uterus and cervix, developing into somatic pain as the perineal structures stretch and distend with discomfort originating from pressure on the pudendal nerves. Translation of these sensations occurs as stimulation reaches the thalamus, brain stem, and cerebellum, hypothalamic and limbic systems, going through a process of transitory analysis with nociceptor impulses then becoming modulated by the central nervous system (Lowe, 2002). The ‘gate control theory’ (Melzack and Wall, 2008) suggests that endorphin release, prompted by certain nerve stimulation, can translate ascending nociceptor information, counter-acting the discomfort experienced and decreasing the intensity of pain (Buckley, 2011; Sanders, 2015). If women acknowledge the hormonal component of birth preparedness, and midwives provide strategies to promote calm and reduce fear, the endogenous hormones necessary for labour to progress smoothly can be increased. This results in women labouring in a conducive environment, avoiding what Foureur (2008) terms ‘the fear cascade’ where adrenaline and catecholamines inhibit oxy tocin, which can contribute to dystocia and maternal distress (Buckley, 2011). Empowering women to be in control of their own birth experience is therefore essential, highlighting the significance of woman-led and self-generated strategies (Karlsdottir et al, 2014).
Water
Water immersion for use in the birth setting has multiple benefits for labouring women, including: enhancing physiological birth (da Silva et al, 2009); reducing use of pharmacology in labour (Eberhard et al, 2005); enhancing maternal feelings of empowerment (Royal College of Midwives (RCM), 2012); and supporting midwifery practices of normality. Since the Changing Childbirth report (Department of Health, 1993), water immersion in labour has been part of national recommendations for low-risk women (Cluett and Burns, 2009). The most recent NICE (2016) guidance recommends that women be offered the ‘opportunity to labour in water for pain relief’, although in practice this can be challenging to facilitate; there is variation in accessibility and availability owing to differences in birthing environment and levels of midwifery confidence. The Birthplace study reported that births in midwife-led free-standing units were four times as likely to occur in water than births in obstetric environments (Birthplace in England Collaborative Group, 2011). Although midwives often achieve competency in facilitating water birth, this skill can require confidence-building if not regularly practised. Part of a wider philosophy of supporting normality, this is arguably most easily achieved in the sphere of physiological birth facilitation most commonly found in midwifery-led environments (Russell et al, 2014; Nicholls et al, 2016). Water immersion can be a useful tool in either the hospital or home setting, enabling women and their partners to self-manage levels of discomfort. Midwifery advice to utilise water in the latent phases of the birth process (Simkin and Ancheta, 2011b; NICE, 2016) may assist women to retain some sense of control and aid maternal feelings of empowerment (Eckert et al, 2001). There is some discussion in the literature about the efficacy of warm showers providing support for negotiating discomfort, with water temperature acting on nerve receptors and decreasing the experience of pain (Benfield et al, 2010). Showering may be a valuable tool for midwives caring for women who do not want to use a birthing pool. This allows for freedom of movement, encouraging regular changes of position that can assist in descent and progress (Simkin and Bolding, 2004; Zwelling, 2010; Lee et al, 2013). This may enhance maternal satisfaction with the birth experience, as well as being cost-effective and appropriate for a wider range of women (Stark and Miller, 2009; Stark et al, 2011).
Complementary and alternative medicines or therapies
As many women seek to avoid pharmacological strategies for pain management in labour, the use of alternative therapies is increasing, with nearly 50% of women of childbearing age accessing complementary and alternative medicine (CAM) (Smith et al, 2006). There is no unified definition of CAMs, but they include ‘complementary and alternative medicine treatments that fall outside of mainstream healthcare’ (NHS Choices, 2016), comprising what the Complementary Medicine Field of the Cochrane Collaboration defines as ‘practices and ideas which are outside the domain of conventional medicine in several countries’ (Berman, 2006). With the increase in access of CAMs by pregnant women in developed countries (Harris et al, 2012), it is important that midwives can support women's choices for labour within the wider practice sphere of national guidance and recommendations (NMC, 2012; 2015). Midwives and their obstetric colleagues recognise that a scientific basis and more professional learning is needed to investigate the role of CAMs in a professional capacity (Mollart et al, 2016). NICE (2016) guidance advises that midwives should not offer or recommend yoga, acupressure or aromatherapy for pain relief in the latent stage of labour, although if women express a desire to utilise these techniques they should be supported to do so.
Relaxation and visualisation
There is an array of relaxation and visualisation techniques that are growing in popularity, promoting and supporting the physiology of birth and a natural approach to pain management. These mind–body techniques include general relaxation and breathing techniques, hypnosis and hypnobirthing, meditation, visualisation and movement. NICE (2016) recommends that midwives may advise women and their birth companions that breathing exercises may assist in decreasing pain during the latent phase of labour. In the current climate of an escalating incidence of analgesia (Whitburn et al, 2014; Leap and Hunter, 2016), limiting these methods to early or latent labour may cause women to look for additional means of negotiating discomfort as birth progresses. This may undermine the woman's ability to birth physiologically, and negate midwives’ skills in facilitating the challenges of labour support.
The Cochrane review of relaxation techniques concluded that relaxation was associated with a reduction of pain intensity in both early and active labour phases (Smith et al, 2011a). Dick-Read (2013) suggests in his seminal work, originally published in 1942, that anxiety and fear cause an increase in pain owing to muscle tension. If the fear–tension–pain syndrome cycle is to be broken, then women must be psychologically at ease without the presence of fear for the impending labour. If they are not relaxed and free from fear, women may experience the aforementioned ‘fear cascade’ (Foureur, 2008), occurring when they feel alone and unsupported (Leap et al, 2010). This can pave the way for catecholamines, cortisol and vassopressins, which disrupt oxytocin production and cause physiological responses owing to maternal distress increasing levels of adrenaline. Fear and adrenaline prompt a ‘fight or flight’ response, resulting in vasoconstriction decreasing oxygenated blood to all non-essential organs, including the uterus (Foureur, 2008; Buckley, 2011; UvnasMoberg, 2011). With the correct antenatal knowledge-sharing between midwives and women, the cognitive process of building up anticipation of pain can be avoided and, rather than negatively assessing their ability to cope with pain (Lumley et al, 2011), women can feel safe and the norms of labour pain become less menacing. The recent use of techniques that formalise breathing and visualisation applied to birth—such as mindfulness and hypnobirthing—may offer women a deeper sense of connectivity with their physical experiences, being fully aware in the present moment.
In Whitburn et al's (2014) exploratory study, women's descriptions of being mindful in labour reported that they could notice pain, accepting it as part of the experience. Although women acknowledged that they were not in control of the pain, they were able to interact with labour sensations while giving them a sense of purpose and focus throughout the process; this allows women to recognise the contribution they make to their own wellbeing (NMC, 2015).
Homeopathy and aromatherapy
Homeopathic remedies are derived from herbs and minerals, with the aim of stimulating the body to achieve equilibrium (Smith et al, 2006). In homeopathy, substances are greatly diluted, and are considered to increase in potency with greater succession (vigorous shaking) and diluting. Their use in the intrapartum setting is dependent on the pain experienced and emotions felt. It has been proposed that the use of homeopathy in labour enables physiological balance and function, soothing and relaxing the woman (Sullivan and McGuiness, 2015; Smith et al, 2006). Despite there being little evidence to support the use of homeopathic remedies in the intrapartum setting, some women may feel that homeopathy is helpful and midwives can facilitate maternal choice and support its use, should women wish.
Aromatherapy is the use of essential oils derived from plants to increase the body's sedative, stimulate and relaxing substances. Essential oils are obtained by distillation and then mixed with a carrier oil such as grapeseed, sweet almond and sesame, although carrier oils can also contain active ingredients such as aloe vera. Oils can be inhaled using steam infusion or a burner, and can also be used in a bath or for massage, which may be particularly effective in the intrapartum environment (Smith et al, 2006; 2011b). Different oils are hypothesised to have different effects, with lavender commonly used in the birthing environment owing to its relaxing and soothing properties, and frankincense used as it is thought to slow and deepen breathing and promote calm (Simkin and Bolding, 2004). Other oils frequently used include eucalyptus and jasmine for reducing pain, clary sage for increasing uterine activity, lemon for elevating mood, mandarin and ylang ylang for relaxation, and rose to reduce anxiety (Tiran, 2000; Smith et al, 2011b).
The mechanism of action for aromatherapy is unclear. Although studies demonstrate no change in physiological parameters, with little evidence to suggest that aromatherapy can alter physiological wellbeing, some studies do suggest an improvement relating to mood and anxiety (Smith et al, 2006; 2011b; Jones et al, 2012; Sullivan and McGuiness, 2015). The use of aromatherapy oils is thought to be harmless, although they may cause skin irritation so patch-testing may be advisable (Tillet and Ames, 2010). Some women may find essential oils unpleasant, and with national guidance indicating that midwives should not offer or advise aromatherapy during the latent phase of labour (NICE, 2016), the importance of being woman-led and supporting women in their choices regarding aromatherapy and homeopathy is essential.
Acupressure and reflexology
There have been a number of studies investigating the efficacy of using acupuncture and acupressure during labour, with results including a reduction in pain experienced, increasing satisfaction of pain management and a reduction in uses of pharmacology (Lee and Ernst, 2004; Smith et al, 2011c) although much conflict remains in the evidence base (Levett et al, 2014). Acupuncture and acupressure are systems based on Chinese medicine (Chen and Wang, 2014) of meridians throughout the body and aim to treat illness and ease discomfort by stimulating acupuncture points, which for labour pain are located in the hands and feet (Smith et al, 2011c). Reflexology is based on stimulating zones and reflex areas on the feet, suggesting these correspond to different parts of the body and that stimulation with gentle manipulation or pressure has been shown to soothe pain, aid relaxation and improve circulation (Ernst and Köder, 1997; Mathew and Francis, 2016). Findings across the literature also suggest that the application of reflexology during labour assists in a reduction of fear, with some suggestion that pain tolerance and threshold can be positively influenced by this technique (Samuel and Ebenezer, 2008).
Data from Smith et al's (2011c) meta-analysis suggest that acupuncture and acupressure may be helpful for women's pain management in labour, but the authors recommend further randomised controlled trials to determine effect and efficacy. There is some suggestion that this type of research is reductionist. It is necessary to take into account practitioner experience, technique variation, birth environment and women's autonomy and position throughout labour. Further research should incorporate the broader context of these supportive techniques (Levett et al, 2014). Much of the literature suggests that women in acupressure control groups experienced a reduction of pain intensity using various pain scales (Chen and Wang, 2014; Levett et al, 2014; Moghimi-Hanjani et al, 2015) with some studies suggesting that the addition of ice combined with massage techniques on pressure points can further decrease pain during birth, giving more persistent painrelief (Hajiamini et al, 2012). Midwives considering the use of acupressure or reflexology for labour will need to balance the fact that they are low-cost and non-intrusive with concerns about safety, efficacy and the current evidence base informing practitioner knowledge (Mollart et al, 2016).
All CAMs must only be used in the best interests of both women and babies and with the appropriate additional training (RCM, 2014). Survey data indicate that many midwives are incorporating alternative and complementary practices into their midwifery care (Pallivalappila et al, 2013). It is important that the individual risks and benefits of each complementary therapy are assessed by midwives, and advice should be offered only within the boundaries of professional accountability by those midwives who have completed additional training, regardless of how the midwife feels about the benefits and efficacy of CAMs (Kenyon, 2009; NMC, 2012). Kenyon (2009) points out that Trust guidance is often only available in units where there are specialist midwives practising who have trained in hypnosis, aromatherapy and specific therapies. Trusts providing protocols about uses of CAMs in pregnancy are able to offer implicit permission for midwives to practise their use under the Trust's vicarious liability insurance, highlighting the need for governance regarding CAMs in maternity services and raising issues of risk-management for both midwives and childbearing women in those units that do not provide such protocols and guidelines (Kenyon, 2009).
Massage and transcutaneous electrical nerve stimulation
Massage therapy during pregnancy and the intrapartum period has long been considered an effective way to relieve pain, reduce stress and anxiety and increase relaxation (Kimber et al, 2008; Field, 2010; Silva Gallo et al, 2013). It is a readily available and easily used strategy for intrapartum pain management. Massage is manipulation of the body's soft tissues, and during the intrapartum period massage techniques in different areas can aid relaxation and soothe the woman (Jones et al, 2012). Massage is ideally individualised to the woman's specific needs during the childbirth continuum. For a woman experiencing lower back ache, lumbosacral massage may be soothing (Jones et al, 2012), whereas for a woman feeling tense and anxious, shoulder massage may enable relaxation. Research suggests that massage in labour is associated with reduced medication use and shorter duration of labour (Field et al, 1997; Field, 2010). The physiology underpinning the efficacy of intrapartum massage is thought to be explained by the ‘gate control theory’. Pain messages are believed to be carried more slowly by C neurons than massage stimulation, which is carried by A neurons, leading massage stimulus to reach the brain quicker and close the ‘gate’ to pain stimulus (Augustinsson et al, 1977; Melzack and Wall, 2008; Field, 2010). Another physiological mechanism underpinning the efficacy of massage suggests that massage leads to increased vagal activity, therefore reducing maternal pulse rate, blood pressure and cortisol levels (Hernandez-Reif et al, 2000; Diego et al, 2004; Field and Diego, 2008; Field, 2010), also improving blood flow and oxygenation of tissues (Vickers and Zollman, 1999). The use of massage can provide the birthing partner with a supportive role in the labouring scenario, thus providing some closeness and intimacy which may enhance maternal satisfaction. Owing to its non-invasive and safe nature, massage is unlikely to have detrimental effects so can be encouraged during the intrapartum period as a method of relaxation. In this way, massage can be considered a useful component of the midwifery pain-management toolkit (Silva Gallo et al, 2013).
Building on the physiological mechanisms underpinning massage, transcutaneous electrical nerve stimulation (TENS) machines are a popular pain-management strategy during the latent and active phases of labour, and have been used in this setting since the 1970s (Augustinsson et al, 1977). TENS is hypothesised to comple ment the release of endogenous endorphins, mediating the experience of pain (Lechner et al, 1991), and may reduce the length of labour by suppressing catecholamine release (Lowe, 2002). Machines consist of a handheld device that controls the frequency and intensity of impulses emitted by connected electrodes, which are applied to the skin of the lower back on either side of the spine (Simkin and Bolding, 2004; Dowswell et al, 2009). Although the efficacy of TENs is widely debated, and evidence is inconsistent as to whether its use reliably reduces uptake of pharmacological pain-management strategies (Dowswell et al, 2009), TENS may enhance feelings of control for some women and provide a distraction from the discomfort of labour, thus alleviating pain and anxiety and improving wellbeing (Simkin and Bolding, 2004; Jones et al, 2012).
Role of the midwife
National recommendations suggest that midwives provide guidance and support, informing women and their birth companions on how to work with any pain experienced, advising women on how to negotiate the latent phase of labour and differentiate between Braxton Hicks and active labour contractions (NICE, 2016). This can be aided by antenatal discussions of the gate theory of pain, enabling women to access strategies that may enhance their confidence. One-to-one midwifery support is associated with a reduction of pharmacological analgesia and increased birth satisfaction (Hodnett et al, 2011), and midwives are ideally placed to empower women to make individual choices to manage discomfort throughout labour. Understanding birth from a physiological standpoint can enable women to feel supported to consider pain during labour not as a problem to be solved, but as a process to be worked through (Leap and Anderson, 2008). Midwives must understand that the very act of offering a ‘pain relief menu’ can unintentionally suggest that women ‘need’ assistance (Leap and Hunter, 2016).
Benefits and drawbacks of each strategy, in light of the woman's emotional wellbeing, physiological clinical picture and birth environment, should be considered throughout intrapartum care. This should be womanled, with the midwife assisting women in choosing the strategy that best suits them at each stage of birth (Enkin et al, 2000). Every birth is unique, and an essential midwifery skill lies in navigating the labour and supporting the woman to feel empowered and in control of managing her pain. This can be particularly challenging when women have labours considered to be high risk, necessitating further monitoring or intervention, as this alters the environment and resources available, such as a birthing pool. In these higher-risk scenarios, the role of the midwife in normalising the complex labour, facilitating normality and advocating for and empowering the woman is vital, and use of the expansive toolkit of non-pharmacological strategies to relax and reduce pain can be hugely beneficial to provide a calm environment.
The RCM (2012) advises that midwives should support all women in using strategies such as breathing, relaxing and changes of maternal position during labour to improve emotional experiences and pain outcomes (Spiby et al, 1999). The psychosocial ramifications of maternal sense of control and satisfaction with pain management in the intrapartum period should not be underestimated, and can have wide-ranging and long-lasting effects on maternal wellbeing and the wider family unit (Carvalho and Cohen, 2013).
Conclusion
As frontline practitioners throughout the childbearing continuum, midwives provide crucial one-to-one support and guidance, with pain management in the intrapartum period being a key area necessitating midwifery expertise. A physiological understanding of the anatomy of birth is key to enable midwives to support women holistically throughout their labour, utilising a toolkit of non-pharmacological pain management strategies to individualise care to each woman throughout her unique journey into motherhood. Working with the physiology of pain is at the forefront of midwifery expertise. Antenatal education and preparation are essential to enable women to approach birth with physiological understanding, and midwives have a responsibility to demystify birth so that women know what function their pain has and what the discomfort they experience is achieving. This midwifery mindset acknowledges that practice requires a more flexible approach to diverse methods, particularly those self-directed and non-pharmacological, in order to facilitate women to have positive experiences (Whitburn et al, 2014).
Key Points
- A physiological appreciation of the natural phenomena of labour is essential to avoid pathologising and medicalising the process
- Midwives can strive to promote normality in all birth settings, individualising care as appropriate
- Midwives should work within the professional remit and individual scope of practice as delineated by the Nursing and Midwifery Council, acknowledging where additional professional development is needed
- Self-generated strategies should be considered ‘gold standard’ to enhance women's empowerment and control
- If women are enabled to appreciate the normality of pain and discomfort within the physiology of labour during the antenatal period, preparedness levels will be enhanced and anxiety and fear can be assuaged

