The overarching aim of midwifery supervision is to ensure that women and their babies receive high-quality and safe care. This goal is enshrined in the Midwives rules and standards (Nursing and Midwifery Council (NMC), 2012). The Midwives rules and standards set out requirements for practice as well as the standards for the Local Supervising Authority (LSA) with regard to supervision and the audit process (rule 7). They include a midwife's responsibility to have her Intention to Practise form signed annually (rule 3: 1); for it to be signed by a named supervisor of midwives (SoM) appointed by the LSA Midwifery Officer (LSAMO) (rule 8) and to undertake an annual review with his or her SoM (rule 9: 1b). The rules and standards also stipulate that each team of midwifery supervisors must be audited annually (rule 7, 2: 1), with the aim of benchmarking each activity to ensure safe practice.
For each supervisory team, the yearly LSA audit provides an opportunity to review initiatives and achievements and to reflect on areas for development or improvement. For reporting purposes, the audit is divided into four domains:
In line with good governance practices of the NMC, each domain is benchmarked by the SoM team against the LSA's standards for the statutory supervision of midwives (LSA, 2014). This informs the framework for the London audit process. As a means of gathering evidence for domains two and three, one London SoM team chose to survey the midwives at their Trust.
Domain two: the profile and effectiveness of statutory supervision
Domain two relates to midwives' experience of supervision, such as the ease of contacting the 24-hour on-call SoM (rule 9: 1d) as well as the availability and supportiveness of their named supervisor. Domain two also relates to rule 9b, which states (NMC, 2012: 26):
‘A local supervising authority must ensure that… at least once a year, a supervisor of midwives meets each midwife for whom she is the named supervisor of midwives to review the midwife's practice and to identify her education needs.’
Domain three: team working, leadership and development
Domain three relates to providing professional leadership and nurturing potential leaders. This function is affected by the ratio of supervisors to midwives, recommended to be 1: 15 (rule 9: 1.2) (NMC, 2012). In London, this ratio currently ranges from 1: 8 to 1: 28 (Read, 2013) and is 1: 19 at the authors' Trust at the time of writing.
Aims
Recent scrutiny of midwifery supervision, particularly the King's Fund report (2015), has revealed that there is a lack of quantifiable evidence on the subject. A systematic literature review concerning midwives' and SoMs' perceptions of statutory supervision was carried out by Henshaw et al (2013). Thirteen of the 19 studies reviewed were published before the 2004 revision of the Midwives rules and standards, which has since been revised again. Even so, Henshaw et al's (2013) findings support the focus and results of this recent survey.
Methods
Questionnaire
For the purpose of the audit domains, the SoM team chose to use a questionnaire as a means of ascertaining midwives' views regarding the effectiveness of supervision; also to better understand whether any midwives would consider applying for the preparation of SoM course. The questions were linked to aspects of supervision described in the rules and standards (NMC, 2012), particularly in relation to domains two and three of the LSA audit.
The team ratified the 10 questions and emailed them as an electronic survey generated via SurveyMonkeyTM. The questions formed an anonymously, self-completed, semi-structured questionnaire. The decision to use 10 questions was partly governed by the restrictions imposed by using the free SurveyMonkeyTM service. However, it was also thought to be a manageable number of questions for midwives to answer in work time.
A link to the survey was sent to 325 midwives at the Trust, including 19 SoMs. Email addresses were obtained through the LSA database (LSAdb). Of the 325 midwives, 58.0% (n=188) responded, of whom eight were SoMs. Using the LSAdb in this way highlighted the features and functions of the LSAdb and how its information may be used. Likewise, it heightened awareness of information governance (LSAMO, 2013a) and the need for supervisees to know what information is on the database and about its use.
The SurveyMonkeyTM questionnaire was open for completion for 10 weeks. An initial email with the link was sent, followed by four reminder emails. Each reminder email reiterated the importance of the midwives' views and notably, following each reminder, the response rate increased. Each email also assured midwives of the anonymity of their responses. At the outset, the authors opted to make use of the free SurveyMonkeyTM service. A consequence of this was that all midwives received a reminder email even if they had already responded to the survey. This caused a degree of frustration to a few but also raised the profile of supervision within the unit in a positive way.
Results and discussion
The survey elicited quantitative (questions 1–8) and qualitative data (questions 9 and 10). The authors reviewed the open questions, individually and then jointly, and used thematical analysis to code and generate the overall themes.
Qualities of a SoM
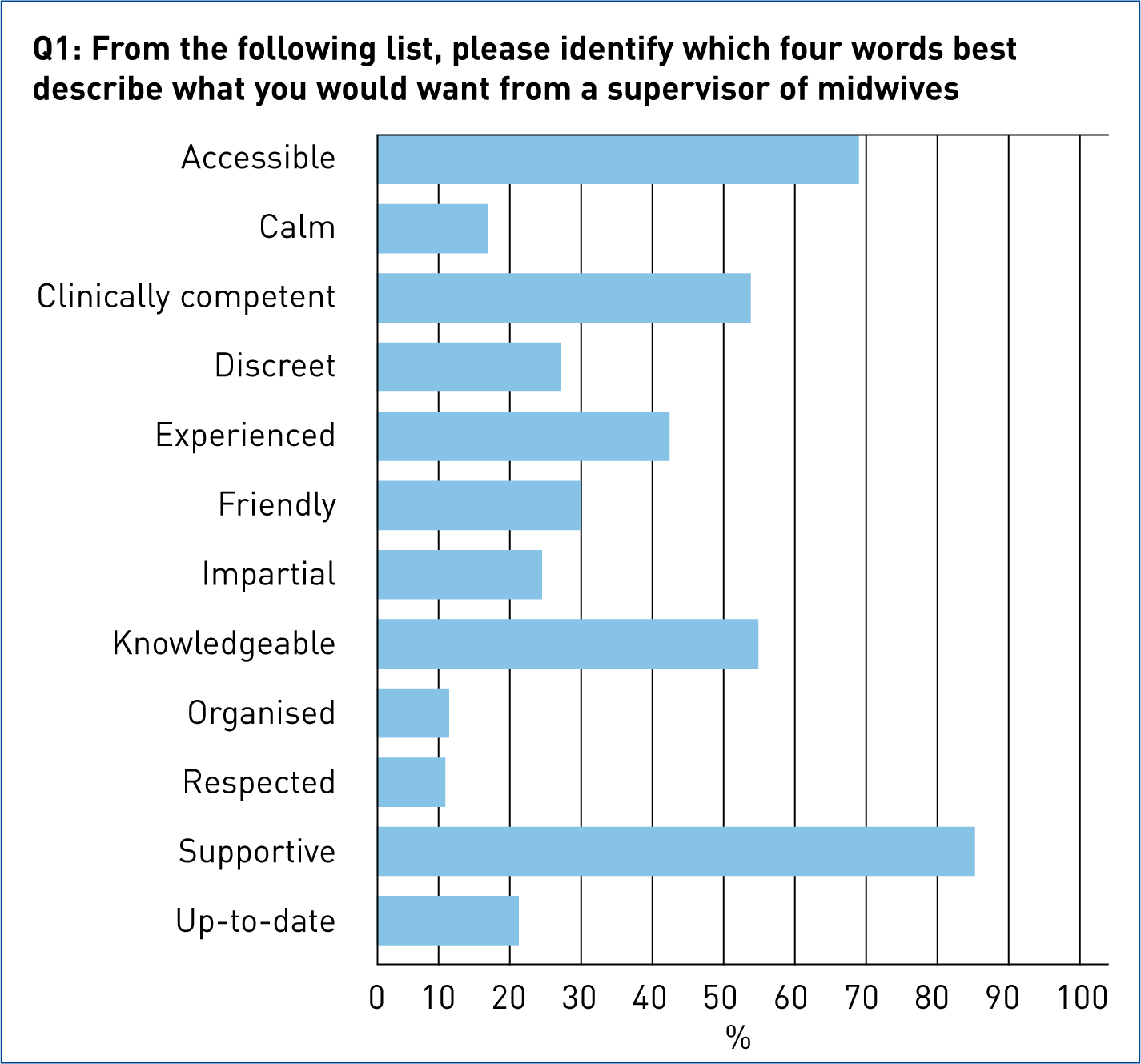
During the annual audit, provision is made for the LSA auditors to speak with midwives working on the day. Often the auditors ask the midwives to describe their named SoM or SoM team. It was decided to adopt a similar format for the first question of the survey. The top four words selected by midwives to describe what they want from their SoM were: supportive, accessible, knowledgeable and clinically competent (Figure 1). In a subsequent questionnaire, it would be useful to compare the answers to this question with the answers to a second question: ‘What top four qualities does your SoM have?’
Accessing a SoM
Questions 2–6 concerned the effectiveness of supervision in relation to accessing a supervisor. Four midwives responded they had never accessed their SoM (question 2). As it is a requirement that every midwife accesses their SoM for an annual review and has their Intention to Practise form signed (NMC, 2012), it may be that this is the response of new starters. However, there are procedures in place for them to meet a SoM on their first day of work. Alternatively, the question may have been inadequately worded.
In relation to question 3: ‘Was it easy to access your SoM?’, four midwives responded ‘not applicable’. Due to the way SurveyMonkeyTM analyses the results, it is not possible to say whether these are the same four who had never accessed their SoM. Of the 5.9% (n=11) who responded that it was not easy to access a SoM, a direct correlation cannot be drawn, but this figure is the same as those who responded that they did not consider supervision at the Trust to be a positive process (question 8).
It was expected that 100% of respondents would answer that Intention to Practise forms and annual reviews were the reason for accessing their SoM (question 4). Surprisingly, the results showed this to be 87.8% (n=165) and 79.3% (n=149), respectively. Positively, 29.3% of respondents (n=56) accessed their SoM for reflection and debriefing (Figure 2).

The finding that midwives frequently access their SoM for reflection and debriefing, along with the other reasons listed in Table 2, corroborates the King's Fund (2015) report that SoMs are mainly involved with ‘regulation via support’. The authors of that report argue this kind of support is beyond the regulatory remit of the NMC. While statutory supervision is debated and discussed with a view to reconfiguration and possibly even renaming (Gillman, 2015), data of this kind are invaluable and worth SoM teams gathering and utilising.
| # | Other (please specify) |
|---|---|
| 1 | Inquest |
| 2 | Challenges in role with other staff member |
| 3 | Inform that the unit is up to capacity |
| 4 | Bullying |
| 5 | Had an incident that occurred at work that involved my supervisor of midwives (SoM) coming to a team meeting at King's College hospital. SoM extremely supportive and drove me to meeting |
| 6 | Agency midwifery on register |
| 7 | Clinical case discussion |
| 8 | Complaint |
| 9 | Bullying by manager |
| 10 | Questions regarding unusual situations |
| 11 | Risk reflection |
| 12 | Support for SoM course |
| 13 | Day-to-day support |
At the authors' Trust, in line with national guidance (LSAMO, 2013b), there is a SoM on-call and a manager on-call in every 24-hour period. This may explain why 62.7% (n=118) of respondents have never accessed the on-call SoM (question 5) and may demonstrate an understanding of the difference between management and supervision. In a future survey it would be useful to ascertain the reasons for calling the on-call SoM, and the practice area of those most frequently doing so.
As noted with question 3, the percentage of people who found it difficult to access the on-call SoM (question 6) is similar to the percentage of people who responded that they do not find the process of supervision positive. As a team, we have had occasional difficulties with our pager system. This may be a contributing factor but is unlikely to be the total explanation.
Changing supervisor
The option to change one's SoM (question 7) is an important tenet of supervision and is assessed during the LSA audit and described in Modern Supervision in Action (LSAMO, 2009). In this survey, 39.0% (n=74) of respondents said they were unsure how, or did not know they were entitled to change SoM. In response to this finding, information has been highlighted through mandatory training and posters displayed in the unit to raise awareness of this option and of the process to follow.
Is supervision a positive process?
When asked directly, 73.4% (n=138) of midwives said supervision is a positive process (Figure 3).
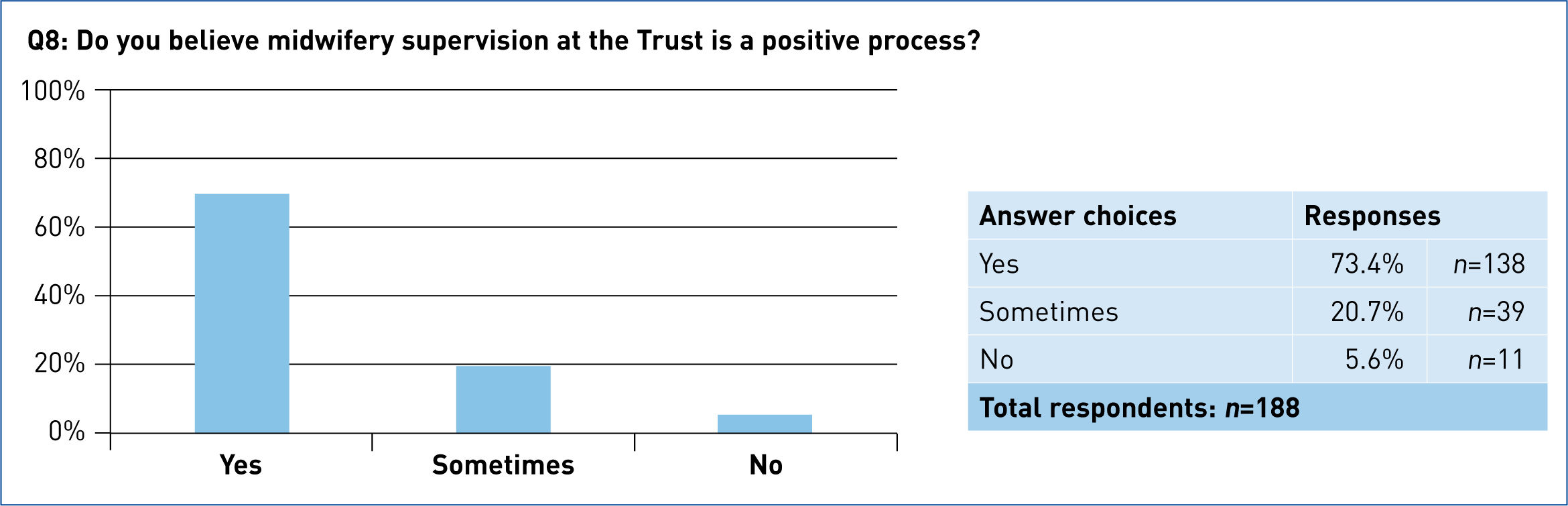
Question nine, a free-text question, aimed to gather qualitative data concerning what makes supervision a positive process. Analysis of the themes revealed that those who found it positive did so because SoMs are supportive, accessible and helpful in providing feedback, which correlates to the answers in questions 1 and 4. Of the 20.7% (n=39) who responded that supervision is ‘sometimes positive’, the main theme was that supervision is variable and dependent on the individual SoM. Of the 5.85% (n=11) who responded that supervision is not a positive experience, this seemed to relate mostly to a poor personal experience of supervision. Examples of the responses given include:
‘I needed to remind my SoM to meet me for my annual review’
‘Often the SoM on-call is the midwife in charge of the shift, I feel like this is a conflict of interest’.
‘I don't believe SoM is useful/necessary as a system to support midwives. I do it because I have to’.
These findings echo that of the systematic literature review conducted by Henshaw et al (2013), which found that the potential for supervision to enhance practice varied according to the nature of the relationship between midwife and supervisor.
Becoming a SoM
Question 10 most directly pertains to domain three of the LSA audit. The purpose was to find out whether midwives had considered becoming a SoM and what factors would dissuade them from doing so. Positively, 31.9% of respondents (n=60) said they would consider becoming a SoM or were in the process of doing so. Analysis of the themes arising from the free-text revealed the following factors influence a person's willingness to do so: experience (enough/not enough), work/life balance including other commitments, insufficient time and apprehension regarding being on-call.
This question was very relevant to the authors' Trust as the SoM: supervisee ratio is currently 1: 19 and has been even greater. During LSA audits, this has been raised as a significant concern and plans made to move towards the recommended 1: 15 ratio. A positive outcome of raising the profile of supervision within the unit through the SurveyMonkeyTM questionnaire was that seven midwives expressed interest in becoming SoMs, of whom four are currently on the SoM course.
In light of recent recommendations to separate the statutory regulatory function from other components of midwifery supervision, the relevance of training future SoMs is a hot topic. However, the Royal College of Midwifery discussion paper, Reframing midwifery supervision (Gillman, 2015: 15) clearly states:
‘The preparation of supervisors is crucial to the success of clinical supervision. Relevant practice experience is important as well as the development of the necessary skills, qualities and characteristics. These include, but are not limited to, active listening, facilitating constructive reflection, mentoring, coaching and enabling practitioners to be outcome focused.’
The obvious follow-on from this is that Preparation of SoM courses must reflect the likely changes in the regulatory aspect of supervision, focusing on the supportive, developmental and leadership end of the current supervisory continuum. These are highly valuable aspects of supervision, as recognised in the King's Fund report (2015).
Evaluation
Using SurveyMonkeyTM to gain midwives’ views of supervision was a worthwhile undertaking and a tool that would be considered for future surveys. The benefit of this method was that, as it is anonymous, midwives appeared to give their honest opinion. Other benefits included results tables and, for a fee, the use of the SurveyMonkeyTM functions. By paying the minimum fee to use the service, email addresses could have been added to the survey to ensure that only midwives who had not responded would receive reminder emails. However, when making this decision, it would be important to check beforehand how many weeks the survey remains open for from the time of payment.
Following completion of the survey and a written audit report, the team of supervisors reflected that this exercise should be repeated in 12–18 months using a similar format to gain women's views concerning the profile and effectiveness of supervision, with the aim of team-working plus developing future leaders. This is particularly pertinent in relation to the recommendations that are currently being considered. For example, little mention is made in the King's Fund report (2015) of the role a SoM can play as an advocate for a woman wishing to plan a birth that goes outside the recommendations of local clinical guidelines.
Conclusion
The findings of this survey demonstrate that the majority of midwives find supervision valuable for professional support. Eliciting the reasons for this, alongside the less favourable comments, is worthwhile for any team of supervisors as it makes it possible to build on what is good and to strengthen other areas for the purpose of providing the safest possible care for women and their babies. In today's climate, when supervision is being scrutinised and critiqued, being able to demonstrate in a concrete way that midwives, and therefore the public, benefit from supervision has become even more vital.

